Why Mammograms Matter
Mammograms are one of the most effective tools available today for early detection of breast cancer — a disease that affects women of many ages and backgrounds. Early detection dramatically improves treatment options and survival rates. For women committed to long-term health and wellness, understanding what mammograms are, when to get them, and how to prepare is essential.
In this article, we explain what a mammogram involves, why it’s important, whom it benefits, when it should be scheduled, and how to interpret the results. We also highlight preparations, limitations, and guidance on follow-up.
What Is a Mammogram?
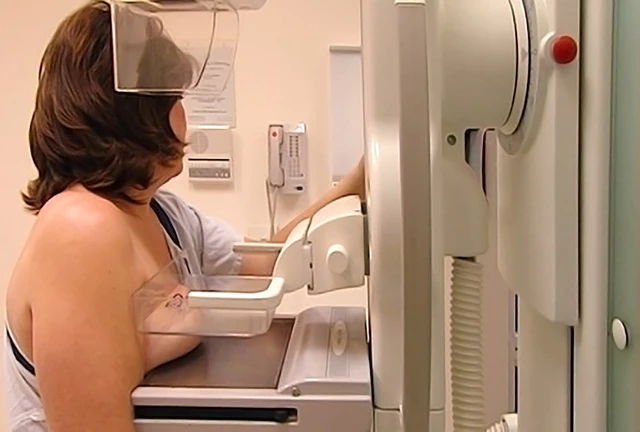
A mammogram is a specialized X-ray imaging technique used to examine the internal structure of the breasts. During the procedure, breast tissue is gently compressed between two plates so that radiographic images can show fine details, such as tissue density or small calcifications, that may otherwise go unnoticed — including potential early signs of tumors or abnormal growths.
Compared to basic physical examination or self-breast checks, mammograms are far more sensitive. Many early-stage tumors cannot be felt by hand but can be detected through imaging — sometimes years before symptoms emerge. Because of this, regular mammograms are considered a cornerstone of proactive women’s health care.
Who Should Get a Mammogram — And When?
Routine Screening for Average-Risk Women
For women without notable risk factors (such as no strong family history of breast cancer or genetic predispositions), clinical guidelines generally recommend beginning routine mammogram screening between ages 40–50, followed by repeat screening every 1–2 years. The exact starting age may vary depending on national recommendations, personal health history, and physician advice.
Earlier or More Frequent Screening for Higher-Risk Women
Women with higher risk — for example, those with a family history of breast cancer, prior breast abnormalities, or certain genetic factors — may benefit from earlier or more frequent screening. In such cases, a doctor may recommend starting mammograms in the late 30s or even earlier, and repeating them annually.
Furthermore, some women may join supplementary imaging protocols (e.g., ultrasound, MRI) in addition to mammograms, under clinical guidance, to maximize early detection—especially when breast tissue is dense.
Key Life Stages to Consider Mammograms
- Perimenopause and menopause: Hormonal changes, increased breast density variability, and age-related risk — mammograms can help monitor changes.
- After childbirth and breastfeeding: Although breast tissue changes naturally, having a baseline mammogram every few years helps track any structural changes over time.
- When beginning hormone therapies or certain medications: Hormonal treatments can influence breast tissue; regular imaging helps monitor safely.
What to Expect During a Mammogram
A mammogram typically takes 10–15 minutes. Here’s what a woman experiencing it can expect:
- Preparation: You’ll be asked to remove clothing from the waist up and wear a medical gown. Avoid applying deodorant, lotion, or powder under the arms or on breasts — these can show up on the X-ray and interfere with image clarity.
- Positioning and Compression: A technologist will position your breast between two plastic plates. The compression may feel firm or mildly uncomfortable, but it lasts only a few seconds — and that pressure helps spread out tissue so the radiologist gets a clear view.
- Image Capture: Usually two images per breast are taken: one top-to-bottom (craniocaudal) and one side-to-side (mediolateral oblique). Additional views may be taken if needed.
- After the Scan: You can immediately go back to normal activities. Some women experience brief mild discomfort or sensitivity, but serious side effects are rare.
Benefits of Regular Mammograms
Early Detection = Better Outcomes
Detecting breast changes before they produce symptoms significantly increases the likelihood of successful, less-invasive treatments. Early-stage cancers detected via mammogram often respond well to therapy — improving survival rates and reducing the need for aggressive treatment.
Monitoring Over Time
With regular mammograms, doctors can track subtle changes in breast tissue over the years — noticing developments in density, calcification, or lumps early on. These incremental patterns often provide critical insights that a single scan cannot.
Peace of Mind and Preventive Care
Even if results are normal, routine mammograms provide reassurance. This not only reduces anxiety about “what ifs,” but motivates continued healthy habits and screenings — a sign of proactive, responsible self-care.
Limitations and Common Misconceptions
While mammograms are powerful, they are not perfect — and understanding their limitations is vital.
- False negatives: Small tumors or those hidden in dense breast tissue may not appear clearly on X-ray. This is more common in younger women whose breast tissue tends to be denser.
- False positives: Mammograms sometimes detect harmless lumps or calcifications that look suspicious, leading to additional tests (ultrasound, MRI, or biopsy) — which may cause anxiety or discomfort.
- Radiation exposure: While the radiation dose during a mammogram is very low — and considered safe — repeated exposure over time still requires responsible scheduling. This is why frequency and necessity must be evaluated with a clinician.
- Not all breast conditions show on mammogram: Some forms of breast cancer (especially very early ductal carcinoma in situ or certain aggressive types) may not appear. That’s why mammograms should be combined with regular clinical breast exams and awareness about self-breast checks.
Because of these limitations, mammograms should be part of a comprehensive breast-health strategy — not the only step.
How to Interpret Mammogram Results
After your mammogram, a radiologist reviews and categorizes the findings, often providing a standard result summary. Common outcomes include:
- Normal / Negative: No signs of abnormal tissue — continue regular screening as advised.
- Benign Findings: Non-cancerous anomalies such as cysts, benign calcifications, or harmless lumps — may require routine monitoring but often no immediate action.
- Suspicious / Abnormal Findings: Areas that need further evaluation — could lead to follow-up imaging or a biopsy.
- Inconclusive / Dense Tissue Warning: Mammogram couldn’t clearly show tissue (common in dense breasts), prompting additional imaging techniques like ultrasound or MRI.
Importantly: an “abnormal” result doesn’t necessarily mean cancer. It means that something needs further investigation. A biopsy or additional imaging often clarifies the situation.
How to Prepare for a Mammogram
To make your mammogram experience as smooth and accurate as possible:
- Schedule optimally: Try to book your mammogram when breasts are least tender — often a week after your menstrual period starts.
- Avoid creams/deodorants: As noted earlier, deodorants, lotions, or powders underarms or on chest can show up as artifacts.
- Wear comfortable two-piece clothes: This makes changing easier at the imaging center.
- Bring previous mammogram images: If you’ve had mammograms before (even at a different clinic), bringing them helps the radiologist compare past and current scans for changes.
- Communicate medical history: Mention any prior surgeries, hormone therapies, breast implants, or family history of breast disease when you register. This context helps tailor imaging or follow-up recommendations.
- Relax and stay still during the scan: Minimizing movement helps produce sharp, usable images.
When to Consult a Doctor Outside of Scheduled Mammograms
While routine mammograms are vital, there are certain situations when you should consult a physician immediately — even if you recently had a normal scan:
- A new lump, swelling, or thickening in breast or underarm area.
- Unusual nipple discharge (especially bloody or clear) or a change in nipple shape or skin texture.
- Persistent pain or discomfort in breast tissue that’s not associated with menstrual cycles.
- Noticeable skin changes — dimpling, reddening, rashes, or puckering of breast skin.
- Family history or genetic predisposition — your doctor may recommend advanced screening earlier or more often.
Early attention to these signs — in combination with regular screening — ensures you stay proactive about breast health.
Making Mammograms Part of a Holistic Women’s Wellness Approach
For a women’s wellness provider like your clinic (e.g. danatalemarat.ae), offering mammogram services — or partnering with trusted radiology centers — should be part of a holistic care approach.
A comprehensive wellness plan for women may include:
- Regular breast-health screenings (routine mammograms).
- Lifestyle guidance — nutrition, exercise, and stress management to support overall wellbeing and reduce cancer risks.
- Patient education — teaching clients about self-breast checks, how to read their bodies, and when to seek medical advice.
- Follow-up care and counseling — for clients with suspicious findings or higher risk, ensuring emotional support and timely referrals.
By integrating mammogram screening into a broader women’s wellness package, your clinic empowers women to take control of their long-term health — combining prevention, early detection, and supportive care.
Myth-Busting: Common Questions and Misconceptions About Mammograms
| Myth / Question | Reality / Answer |
| “I’m too young for breast cancer — I don’t need a mammogram.” | While risk increases with age, younger women — especially with family history — can also develop breast abnormalities. Discuss your risk factors with a doctor. |
| “Mammograms are painful, so I’ll skip them.” | Discomfort during compression is brief. The temporary squeeze helps get clear images — and the benefit of early detection outweighs momentary discomfort. |
| “If my mammogram came back normal, I don’t need to do self-breast checks.” | Mammograms improve detection, but they don’t catch everything. Self-exams and clinical breast exams remain important between screenings. |
| “Dense breasts mean I don’t need mammograms — I’ll just rely on ultrasound.” | Ultrasound can be helpful, but mammograms remain the standard screening tool. For dense breasts, both may be recommended for best results. |
Mammograms as a Cornerstone of Women’s Health
Mammograms are more than just another health appointment — they are a proactive step toward long-term wellness, early detection, and peace of mind. For many women, especially those above 40 or with risk factors, regular mammograms can make all the difference.
By understanding how mammograms work, when to get them, how to prepare, and how to respond to results, women can better advocate for their own health. When combined with a broader wellness approach — including nutrition, lifestyle, education, and emotional support — mammograms play a critical role in comprehensive care.
For clinics like yours, offering reliable, well-communicated mammogram screening and follow-up services is an essential part of a holistic women-wellness offering.